How to Increase Bone Density (& Best/Worst Exercises For It)
Listen to the podcast version of this article.
“Bones are dynamic structures that respond to stress and require both nutrients and activity to maintain strength and density.”
– Harvard Medical School
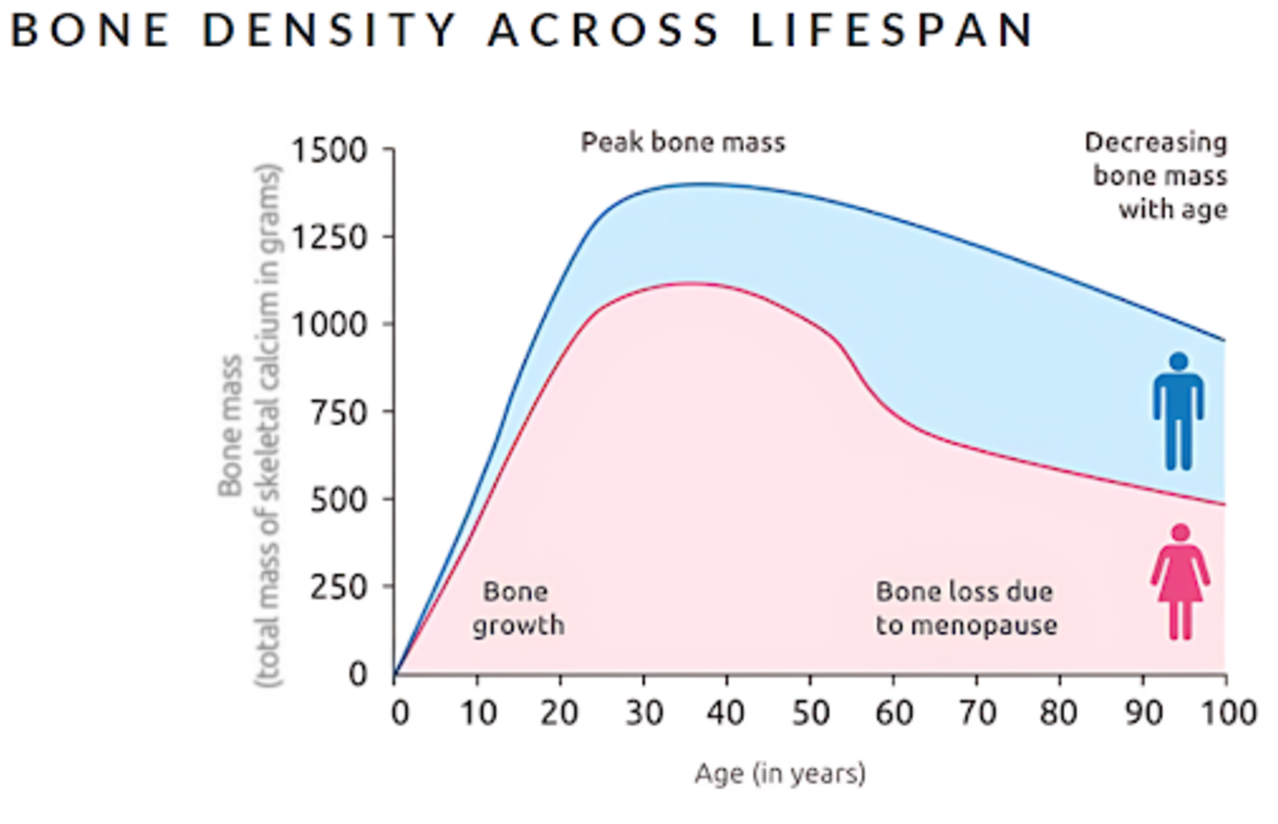
Did you know that up to 50% of women and 20% of men over 50 will break a bone due to osteoporosis? It’s a staggering statistic, but the surprising part is that osteoporosis doesn’t start in old age—it’s often considered a “disease of childhood.” That’s because the foundation for strong bones is built early in life, with peak bone mass typically reached by age 30. After that, maintaining bone density becomes a game of preservation rather than growth.
Whether you’re focused on protecting your child’s future or preserving your own bone health, every decision matters. From the foods you eat to the exercises you choose, your daily habits either strengthen or weaken your skeleton. The good news? It’s never too early—or too late—to start taking action. The steps you take today can build resilience, prevent fractures, and ensure you stay strong well into old age.
The Physiology of Bone
Bones aren’t static—they’re living, dynamic tissues constantly adapting to the demands placed on them. Two key players manage this process: osteoblasts, which build bone, and osteoclasts, which break it down. Mechanical loading—such as weight-bearing activities—stimulates osteoblast activity, leading to increased bone mineral density (BMD) and enhanced bone strength.
This response is governed by the mechanostat theory, which posits that bones adapt to the forces they experience. The greater the load applied, the more bone is deposited to resist future strain. The reverse is also true—when bones aren’t loaded with mechanical stress, they weaken over time. This is why staying active is essential for maintaining bone health and preventing conditions like osteoporosis (a condition where bones become weak and prone to fractures) and osteopenia (a precursor to osteoporosis characterized by lower-than-normal bone density).
Bone Development from Birth to Adulthood
Bone development, also known as ossification, begins before birth and continues into early adulthood. The process occurs in two main forms: intramembranous ossification (direct bone formation) and endochondral ossification (where cartilage is replaced by bone tissue).
During early life, peak bone mass is accrued, typically reaching its maximum by the age of 20-30. This period is critical as it establishes the foundation for lifelong skeletal health.
Osteoblast and osteoclast activity is balanced in healthy bones, but hormonal changes, nutritional factors, and mechanical stress can influence this balance. Sex hormones like estrogen and testosterone play pivotal roles in regulating bone density. Women, especially post-menopause, experience a decline in estrogen, which accelerates bone loss. Men, although also affected by aging-related bone loss, generally retain more bone mass due to sustained testosterone levels. Optimizing bone development during childhood and adolescence is vital, as the bone mineral content (BMC) achieved during these years serves as a "bone bank" for the future.
Bone development begins in the womb and accelerates during childhood and adolescence, with peak bone mass typically achieved by age 30. Think of this phase as a “bone bank”—the more you deposit early in life through proper nutrition, physical activity, and healthy habits, the better equipped you’ll be to weather the natural bone loss that occurs with age. During this critical period, calcium and Vitamin D are indispensable. Calcium is the main building block of bones, while Vitamin D ensures your body can absorb and utilize it effectively. Combined with high-impact activities like running, jumping, or playing sports, these nutrients lay the foundation for lifelong skeletal health.
Optimizing Children’s Bone Health
Building strong bones early is critical for lifelong bone health. To optimize your child’s bone development, focus on three key areas: nutrition, sunlight exposure, and physical activity.
Nutrition
What we eat plays a foundational role. Protein, Calcium, and Vitamin D are essential nutrients for developing a strong skeletal structure.
Calcium is the primary mineral that makes up bone tissue, while Vitamin D facilitates calcium absorption from the gut. For optimal bone health, children should consume calcium-rich foods like dairy products, leafy greens, and seafood.
Vitamin D should be mainly sourced from sun exposure, as well as foods like fatty fish and mushrooms and supplementation if a blood test indicates low levels.
Protein is also vital for bone growth and development in children, as it provides the building blocks for collagen, a key component of bone structure. Ensure your child gets enough protein through whole foods with sources like lean meats, dairy, eggs, legumes, and nuts.
Sunlight
Exposure to the sun is the best natural source of Vitamin D. About 10-30 minutes of direct sunlight several times per week (directly and not through a window) is generally adequate for most children, but this varies with skin type, location, and season. This natural synthesis of Vitamin D is critical for ensuring proper bone mineralization and overall growth. See below for how to know if you’re getting enough vitamin D.
Physical Activity—The Best
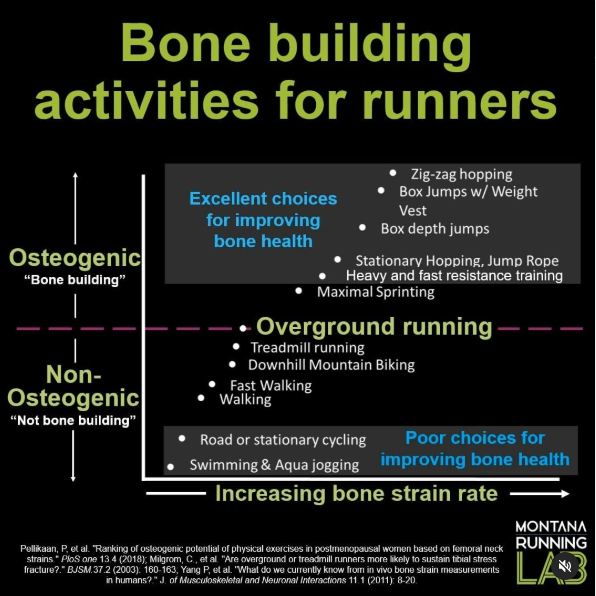
Physical activity is a critical driver of bone accrual during childhood and up through your 20s. Weight-bearing and impact-loading exercises are the most effective for building bone strength because they are osteogenic (“bone-building”). These activities stimulate osteoblast activity, which increases bone mineral density (BMD) and strengthens the skeleton.
Best Sports for Bone Health
Basketball
Gymnastics
Tennis
Soccer
Volleyball
Martial Arts
Best Exercises for Bone Health
Sprinting
Plyometric movements (depth jumps, jumpies, side-to-side pogos, etc.)
The outdated myth that strength training damages growth plates has been debunked. In fact, resistance and impact exercises are essential for building stronger muscles and bones, promoting long-term skeletal health.
Physical Activity—The Worst
Sedentary behaviors, such as excessive screen time (phone, TV, video games), are the worst for bone health as they provide no mechanical stimulation to strengthen bones. Even some physical activities, while beneficial for other aspects of health, are considered non-osteogenic (“non bone-building”) because they lack the impact loading needed to increase bone density.
Least Effective Activities for Bone Health
Swimming
Aqua jogging
Cycling
Rowing
Walking
Treadmill running
While any activity is better than none, these options don’t provide sufficient stress on bones to stimulate osteoblast activity. Even running, while traditionally thought of as impactful because of the “pounding,” may not be as effective for bone-building as once thought due to the body’s ability to efficiently absorb shock while running.
Corticosteroid Use
Corticosteroid use in children, often prescribed for conditions like asthma or autoimmune disorders, can negatively impact bone health. These medications alter the balance between osteoblasts (bone-building cells) and osteoclasts (bone-resorbing cells), leading to decreased bone formation and increased bone breakdown. Long-term corticosteroid use can lead to glucocorticoid-induced osteoporosis (GIO), putting children at higher risk for fractures and slowed bone growth. It’s crucial to work closely with your healthcare provider to explore alternative therapies, appropriate dosages, and, if corticosteroids are necessary, ensure regular bone health monitoring with DEXA scans. In such cases, reinforcing other bone-strengthening habits—like physical activity and proper nutrition—becomes even more important.
Preserving Bone Density in Adulthood
Bone density naturally declines with age, but it’s important to implement strategies to preserve bone mass and prevent osteoporosis later in life regardless of age. Here’s how to slow the process of bone loss:
Physical Activity
Continue to include movements and exercises that are osteogenic into your routine (see above).
Nutrition: Protein, Calcium, & Vitamin D
Calcium: Continue to get enough calcium, prioritizing whole foods. See above for more.
Vitamin D: Continue to get enough Vitamin D through whole foods, sunlight, and, if necessary, supplementation.
Sunshine: Direct sunlight is the best for you health and Vitamin D levels but if you live above the 37th parallel then you are not able to get enough Vitamin D from November to March. The rule of thumb is that if your shadow is longer than you are tall then you’re not making much or any Vitamin D. The DMinder app is great at telling you if you’re getting enough sun and when to get the best bang for your buck (Android, iOS). This “Sunshine Calendar” can also give you a general idea of your seasonal sun dosage potential.
Supplement: Vitamin D3 is the most effective form, and it’s best absorbed when paired with Vitamin K2 to ensure calcium is directed to your bones and not your arteries. Consider a supplement (this is a good third-party tested one with D3+K2) during the darker months. I take one from about Halloween to St. Patrick’s Day to maintain optimal levels.
SAD/Happy Lamp: Another strategy I use during these darker months is using a SAD Light Therapy Lamp in the mornings for about 20 minutes.
Protein: Protein plays a critical role in preserving bone density as it provides the amino acids necessary for collagen synthesis, a major component of bone structure. Adequate protein intake has been shown to improve bone mineral density and reduce fracture risk, especially in older adults. Aim for at least the minimum effective dose of 0.82 grams of protein per pound of desired body weight per day (1.8 grams per kilogram). While high-quality whole foods are the best source, I use these strategies when I know I won’t hit this minimum for the day:
Protein bars (my favorite is IQBar)
Jerky (go with a grass-fed version)
Protein powder (I use Levels Grass-Fed 100% Whey Protein because it comes from grass-fed cows among other benefits).
Lifestyle Modifications
Avoiding smoking, limiting alcohol intake, and managing stress to protect bone health. In addition to creating inflammation, smoking reduces blood flow to bones, and alcohol interferes with calcium balance, contributing to weaker bones over time.
Bone Loss During Menopause and Strategies for Women
The transition into menopause marks a significant period of bone loss for women, primarily due to a sharp decrease in estrogen levels, which plays a protective role in bone metabolism. Women can lose up to 20% of their bone density in the first five to seven years after menopause, increasing their risk of osteoporosis and fractures.
Hormone Replacement Therapy (HRT): Estrogen replacement is effective in slowing post-menopausal bone loss. While HRT can be beneficial for bone density, it is important to weigh the risks and benefits with a healthcare provider due to potential side effects like increased risk of cardiovascular disease and breast cancer.
Physical activity: High-impact and resistance-based exercises are critical for maintaining bone density. Post-menopausal women should prioritize weight-bearing activities, such as strength training, to stimulate bone formation.
Dietary interventions: Adequate calcium and Vitamin D intake continues to be crucial during and after menopause. For women at higher risk of osteoporosis, physicians may also recommend bisphosphonates or other medications that help prevent bone loss. Talk to your doctor.
Interpreting a DEXA Scan
A Dual-Energy X-ray Absorptiometry (DEXA) scan is the gold standard for assessing bone mineral density (BMD). The results provide a clear picture of bone health and fracture risk, with two key metrics used to interpret the data: T-scores and Z-scores.
T-score: This value compares an individual’s BMD to that of a healthy 30-year-old adult. A T-score of -1.0 or higher is considered normal, -1.0 to -2.5 indicates osteopenia (low bone mass), and -2.5 or lower signifies osteoporosis.
Z-score: This value compares a person's BMD to what is expected for their age, gender, and size. A Z-score below -2.0 is considered low for age, signaling that factors other than aging (e.g., medical conditions or medications) may be contributing to bone loss.
Understanding these scores is essential for determining a treatment plan. A low T-score may prompt lifestyle changes, while a significantly low Z-score might require a more in-depth investigation to identify underlying causes of bone weakness.
Takeaway
Your bones are living, dynamic structures, constantly adapting to the forces and nutrients you give them. Think of them as a long-term investment: every healthy habit you adopt now is a deposit into your “bone bank” for the future. Prioritize high-impact, weight-bearing exercises like basketball or resistance training, which stimulate bone-building cells called osteoblasts and improve bone mineral density.
Make your diet work for you by including calcium-rich foods, Vitamin D from sunlight and food, and adequate amounts of prottain Beyond that, cut back on habits that weaken bones, such as excessive screen time, smoking, or drinking too much alcohol.
Finally, remember that your bones thrive on variety and consistency. Whether you’re jumping rope with your kids, adding weight to your squats, or simply spending time in the sun, each action builds a stronger foundation. Stay proactive and intentional, and you’ll not only improve your bone density but also safeguard your mobility and independence for years to come.
FAQ
At what age should I start focusing on bone health?
Bone health is important at every age. Peak bone mass is typically reached by age 30, so childhood and young adulthood are critical periods for building bone density. After 30, the focus shifts to preserving bone mass and preventing loss.
How much calcium do I need for healthy bones?
Adults typically need around 1,000 mg of calcium per day, increasing to 1,200 mg for women over 50 and men over 70. Get calcium from whole foods like dairy, leafy greens, and fortified products.
How does Vitamin D affect bone health?
Vitamin D helps your body absorb calcium and plays a critical role in bone mineralization. Without enough Vitamin D, your body can't effectively use calcium, leading to weakened bones.
What’s the role of protein in bone health?
Protein is essential for bone health because it provides the building blocks for collagen, a key component of bone structure. Aim for at least 0.82 grams of protein per pound of desired body weight per day for optimal bone density and muscle support.
How can I check my bone density?
A Dual-Energy X-ray Absorptiometry (DEXA) scan is the gold standard for measuring bone density. It provides T-scores and Z-scores to assess bone health and fracture risk.
Can I reverse bone loss?
While you can't fully restore lost bone density, you can slow or stop further loss with weight-bearing exercises, proper nutrition (calcium, Vitamin D, protein), and lifestyle changes like avoiding smoking and limiting alcohol.
Should children do specific exercises for bone health?
Yes, children benefit from weight-bearing and high-impact activities like jumping, sprinting, and sports. These activities help build peak bone mass, which serves as a "bone bank" for their future.
Are supplements necessary for improving bone density?
Supplements may be helpful if your diet lacks key nutrients like calcium, Vitamin D, or protein. Always consult your doctor to determine what supplements, if any, you need.
How quickly can I see improvements in bone density?
Bone density changes gradually. With consistent exercise, proper nutrition, and healthy habits, you may see improvements over several months to years, depending on your starting point. Regular DEXA scans can track progress.
Related: